Category: Medicine
Paging Dr. Siri
In 2004 I wrote In Praise of Impersonal Medicine arguing:
I have nothing against my physician but I would prefer to be diagnosed by a computer. A typical physician spends most of the day playing twenty questions. Where does it hurt? Do you have a cough? How high is the patient’s blood pressure? But an expert system can play twenty questions better than most people. An expert system can use the best knowledge in the field, it can stay current with the journals, and it never forgets.
and in 2006 I noted:
The practice of modern medicine is surprisingly primitive…My credit card company knows far more about my shopping history than my physician knows about my medical history.
I now believe that we are on the cusp of major changes to medicine. The thousand dollar genome sequence is less than a year away, Ford has just developed a car seat that can monitor your health, many people are already using wrist monitors to measure heart and sleep patterns. All of this data will soon be combined with massive databases to offer predictive and prescriptive health diagnosis.
In Do We Need Doctors or Algorithms the venture capitalist Vinod Khosla expands:
IBM’s Watson computer… is now being applied to medical diagnosis after handling imprecise and vague tasks like winning at Jeopardy, which experts a few years ago would have said could not be done. “Computers cannot match the judgment of humans on these kinds of tasks!” And with enough data, medical diagnosis or 90% of it is an easier task than Jeopardy.
Already Kaiser Permanent already has 10 million real-time medical records with details of 30,000,000 e-visits last year with caregivers and computer modeling of key diseases per individual that data scientists would love to get their hand on. Already, according to IDC 14% of the US population is using their phones for medical help and 200 million health and fitness related mobile applications have been downloaded according to pyramid research. Fun stuff, though early. They are probably two generations away from systems that are actually useful.
…But I doubt very much if within 10-15 years (given continued investment and innovation and keeping the AMA from quashing such efforts politically) I won’t be able to ask Siri’s great great grandchild (Version 9.0?) for an opinion far more accurate than the one I get today from the average physician. Instead of asking Siri 9.0, “I feel like sushi” or “where can I dispose a body” (try it…it’s fairly accurate!) and with your iPhone X or Android Y with all the power of IBM’s current Watson computer in the mobile phone and an even more powerful “Nvidia times 10-100” server which will cost far less than med school with terabytes or petabytes of data on hundreds of millions (billions?) of patients, including their complete genomics and proteomics (each sample costing about the same as a typical blood test).
No-give, No-take in Israel
In Entrepreneurial Economics I argued for a “no give, no take” system for organ donation–people who signed their organ donor cards would be given priority over non-signers should they one day need an organ. The idea has an element of justice to it but the primary goal is to increase the incentive to sign one’s organ donor card.
Israel recently adopted this policy by giving extra points on the allocation system to people who previously signed the organ donor card. In the case of kidneys, for example, two points (on a 0-18 point scale) are given if the candidate had three or more years previous to being listed signed their organ card. One point is given if a first-degree relative had signed and 3.5 points if a first-degree relative had previously donated.
It’s early but so far the policy appears to be very successful:
Due to the population’s surge of interest in obtaining an organ donor card, the Adi-National Israel Transplant Center has extended through March 31 the deadline to register as a donor and receive special benefits.
…During the past few weeks, Adi’s phone system has collapsed several times due to the high demand.
Since Adi decided to give preferential treatment to those registering as a potential organ donor, tens of thousands of people have registered, raising the number of potential donors to over 600,000. Until last year, the rate of registration was among the lowest in the Western world.
Hat tip to David Undis whose excellent group Lifesharers (I am an adviser) is implementing a private version of no-give, no take in the United States.
Here is my piece on Life Saving Incentives and here are previous MR posts on organ donation.
Not anomalous enough
This is from an article about the transmissibility of bird flu:
But there have also been some anomalous cases, including a group of diners in Vietnam who apparently were infected by raw duck blood pudding, and the handlers of fighting cocks who were stricken after sucking blood and mucus out of their birds’ beaks.
What went wrong with U.S. health care cost control?
So if the real problem with U.S. health spending is that the U.S. diverged from its peer countries for a decade-long stretch, solving that problem isn’t quite as simple as mimicking the institutions and strategies of our peer countries, whether it’s Canada’s single-payer system or the hybrid models of France or Germany. Our peer countries are facing the same challenges we are, albeit with slightly more breathing room.
This raises the question of what exactly changed in the 1980s. Daeho Kim, a graduate student at Brown University, offers a provocative hypothesis in a new working paper. As Kim explains, a 1983 Medicare reform created the prospective payment system, or PPS, which offered fixed reimbursements for the use of a medical technology. If a physician decides to use bypass surgery as a cardiac treatment, she won’t be paid on the basis of what it cost her to perform the surgery. Instead, she’ll be paid the national average cost. This way, there is a strong incentive to beat the national average cost of performing bypass surgeries, thus lowering, in theory, systemwide costs.
But something quite different seems to have happened. A big part of the story is that providers can choose from a number of different cardiac treatments, some of which are more expensive than others. PPS encouraged them to focus on the treatments where the marginal cost — the cost of providing one more treatment, in this case — fell below the average cost, even if there are more cost-effective treatments available. Kim suggests that PPS may account for one of the most distinctive aspects of the U.S. health system — our extraordinarily overreliance on costly treatments. If Kim is right, it is the failure of bureaucratic price-setting, not the failure of market competition, that may have supercharged health inflation in the 1980s and beyond.
That is from Reiham Salam. I will read through the Kim paper carefully and perhaps report back on it. This is an important topic.
Ask the boss
Nicolas Sarkozy, French president, on Friday outlined what he expected would happen as a result of the central bank’s move.
“Italian banks will be able to borrow [from the ECB] at 1 per cent, while the Italian state is borrowing at 6-7 per cent. It doesn’t take a finance specialist to see that the Italian state will be able to ask Italian banks to finance part of the government debt at a much lower rate.”
The article is here. My earlier comments, sadly neglected by an otherwise attentive blogosphere, were here.
Medical Patents Must Die
Prometheus gave man fire, thankfully he didn’t charge every time man lit a match. Prometheus Labs in contrast wants to charge patients for a rule that says when to increase or decrease a drug in response to a blood test. Quoting Tim Lee:
The patent does not cover the drug itself—that patent expired years ago—nor does it cover any specific machine or procedure for measuring the metabolite level. Rather, it covers the idea that particular levels of the chemical “indicate a need” to raise or lower the drug dosage.
Even this is not quite right for suppose a physician notes that the patient’s metabolites are within the range where a change in dosage is not necessary; although the physician takes no action she still has used the patent and thus must pay Prometheus Lab a fee or infringe.
We already have significant incentives for producing pharmaceuticals (and thus the instructions required to best use those pharmaceuticals), we support medical research through universities and non-profit hospitals, and there is plenty of opportunity to profit from the manufacture of tests. Will we really get enough additional innovation to justify the monopoly prices and deadweight losses when we enforce patents on medical rules? Remember, we have to pay the higher prices on all the rules not just the ones brought into being by the patent.
And if medical patents why not economic patents? Will Scott Sumner now patent a rule for adjusting the money supply in response to metabolites the futures market? 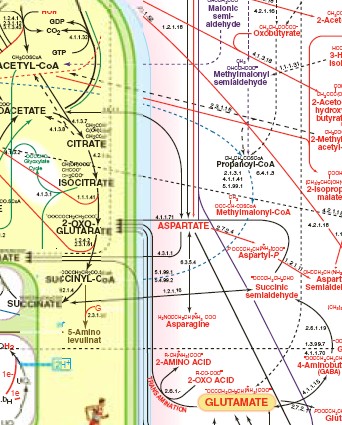
Patents like this are a logical consequence of the extension of patentable matter to software and business methods but extending patents to software and business methods has created huge legal costs without any increase in innovation.
Most importantly, patents can reduce innovation and are especially likely to do so in fields where innovations build on innovations. In fields of cumulative innovation, previous patents owners become veto players who can threaten to holdup the new innovation unless they are granted a share of the proceeds. In theory, bargaining can result in an efficient outcome. In practice, it means lawsuits, delay, waste and reduced innovation.
Since a smartphone may rely on many thousands of previous patents, the smartphone industry has heretofore been considered a classic case of how too many veto players can impede innovation. But now consider human metabolism, one of the most complicated systems known to man (just a tiny fraction of that system is shown at right), and note that if Prometheus is successful in this lawsuit that any correlation in that system can be patented. This is a recipe for disaster.
Addendum: Scotus Blog has a roundup of links. See Launching the Innovation Renaissance (Amazon link, B&N for Nook, also iTunes) for more on patents and their problems. Hat tip also to E.D. Kain who writes:
The world, it appears, is determined to turn me into a full-fledged libertarian. What with SOPA, PIPA, the NDAA, software patent trolling, police violence, and now patents on how doctors provide treatment to their patients, it’s becoming more and more clear how pernicious the law can be when it’s designed for powerful special interests, national security hawks, and big corporations.
Organ Donors for Compensation
Today Alexander Berger will donate a kidney:
NYTimes: On Thursday, I will donate one of my kidneys to someone I’ve never met. Most people think this sounds like an over-the-top personal sacrifice. But the procedure is safe and relatively painless. I will spend three days in the hospital and return to work within a month. I am 21, but even for someone decades older, the risk of death during surgery is about 1 in 3,000. My remaining kidney will grow to take up the slack of the one that has been removed, so I’ll be able do everything I can do now. And I’ll have given someone, on average, 10 more years of life, years free of the painful and debilitating burden of dialysis.
Alexander doesn’t want any praise or talk of “heroic sacrifice,” that is part of the problem. He wants to normalize donation and he argues for compensation in a regulated market.
The people waiting for kidneys aren’t dying because of kidney failure; they’re dying because of our failure — without Congress’s misguided effort to ban organ sales, they would have been able to get the kidneys they desperately needed.
…There’s no reason that paying for a kidney should be seen as predatory. Last week, the Ninth Circuit Court of Appeals issued a ruling legalizing compensation for bone marrow donors; we already allow paid plasma, sperm and egg donation, as well as payment for surrogate mothers. Contrary to early fears that paid surrogacy would exploit young, poor minority women, most surrogate mothers are married, middle class and white; the evidence suggests that, far from trying to “cash in,” they take pride in performing a service that brings others great happiness. And we regularly pay people to take socially beneficial but physically dangerous jobs — soldiers, police officers and firefighters all earn a living serving society while risking their lives — without worrying that they are taken advantage of. Compensated kidney donors should be no different.
Here are further MR posts on organ donation and here is Jon Diesel on Do Economists Reach a Conclusion on Organ Donation.
Rewarding Altruism: Blood for Money
Do pecuniary incentives increase blood donation or do extrinsic incentives crowd out intrinsic incentives? In Rewarding Altruism (NBER, free) an important and impressive new paper Nicola Lacetera, Mario Macis and Robert Slonim analyze a field experiment involving some 100,000 donors and find that pecuniary incentives significantly increase blood donations. The field experiment covers a wide geographic area and the donors are tracked for a significant period of time after donating so the authors can look for geographic and temporal spillovers. The authors offered potential donors gift cards of $5, $10 and $15.
Subjects who were offered economic rewards to donate blood were more likely to donate, and more so the higher the value of the rewards. They were also more likely to attract others to donate, spatially alter the location of their donations towards the drives offering rewards, and modify their temporal donation schedule leading to a short-term reduction in donations immediately after the reward offer was removed. Although offering economic incentives, combining all of these effects, positively and significantly increased donations, ignoring individuals who took additional actions beyond donating to get others to donate would have led to an under-estimate of the total effect, whereas ignoring the spatial effect would have led to an over-estimate of the total effect.
Some of the increase in supply came from temporal substitution but this is not without value. Incentives are not just about increasing supply but also about increasing supply at the right time, i.e. when blood is most needed so it’s useful to have a lever that can influence when donations are made.
Crowding out did receive some support in an odd context. The authors found that donors who were surprised with a gift card after they had donated were less likely to donate in the future. Thus, the donors did not reciprocate the unexpected gift and may have felt that their altruistic intention was being undermined. Once again we see the overwhelming importance of context when trying to understand incentives. To paraphrase Mises, an incentive is not an objective fact but a subjective interpretation.
The authors did not find any decline in quality ala Titmuss. Indeed, this is to be expected since modern blood donation is not a random shout-out to people on the street but instead relies predominantly on repeat donors with a long donation history.
Gift cards of $5, $10 and $15 are small incentives and the authors suggest that the benefits from the increased supply far exceed the costs. It’s notable that it takes longer to donate blood plasma and as a result the U.S. blood plasma industry (the “OPEC of blood plasma”) has always relied on paid donors.
Here are my powerpoint slides on Incentives to Increase Organ Donation and here is an older post on sperm exports.
Jonathan Gruber’s *Health Care Reform*
It is a new graphic novel, by Gruber, illustrations by Nathan Schreiber, and it covers the U.S. health care system and ACA. Excerpt:
Everyone will be able to afford insurance.
You won’t have to worry about going broke if you get sick.
We will start to bring the cost of health care under control.
And we will do all this while reducing the federal deficit.
Claims about health care
The magnitudes of our empirical findings imply that changing provider incentives explain up to one third of recent growth in spending on physician services. The incremental care has no significant impacts on mortality, hospitalizations, or heart attacks.
That is from Joshua D. Gottlieb, who is on the job market this year from Harvard.
Compensation Now Legal for Bone Marrow Donation
Excellent news; yesterday the Ninth U.S. Circuit Court of Appeals issued a unanimous opinion stating that compensation for bone marrow donation, specifically peripheral blood stem cell apheresis, is legal because such donation does not fall under the National Organ Transplant Act (NOTA).
The case was simple and it’s outrageous that the government fought. In brief, a bone marrow donation used to require inserting a very big needle into the donor’s hip bone, a painful hospital-procedure often requiring general anesthesia. Today, however, donors typically do not donate marrow but hematopoietic stem cells which can be harvested directly from blood in a procedure that takes a little longer but is essentially similar to a standard blood donation. Compensation for blood is legal (blood is excluded as an organ under NOTA). The plaintiffs, led by the Institute for Justice, argued and the court agreed that there is no rational basis for outlawing one type of blood donation when a similar donation is legal.
I was shocked by the utter boneheadedness of one of the government’s arguments:
…the government argues that because it is much harder to find a match for patients who need bone marrow transplants than for patients who need blood transfusions, exploitative market forces could be triggered if bone marrow could be bought.
In other words, markets are forbidden just when they are most useful. It was in fact the patients with rare matches who brought this case. As the court noted:
…a physician and medical school professor…says that at least one out of five of his patients dies because no matching bone marrow donor can be found, and many others have complications when scarcity of matching donors compels him to use imperfectly matched donors. One plaintiff is a parent of mixed race children, for whom sufficiently matched donors are especially scarce, because mixed race persons typically have the rarest marrow cell types.
The patients with the most common cell types can afford to rely on the kindness of strangers. You don’t need a lot of kindness when there are a lot of strangers. The patients who are most difficult to match need to leverage altruism with incentive. It’s a lesson with many applications.
From the comments (pleasing David Wright)
There seem to be an awful lot of arguments floating around the economic blogosphere lately that try to use “credibility” as a kind of magic trick to claim that some institution can get some desired result without having to do the yucky things it would have to do to, you know, actually get that result. I would love to see a post on this topic from our host.
That was from David Wright…and now he has his post.
Small samples mean statistically significant results should usually be ignored

Genomes Unzipped: In October of 1992, genetics researchers published a potentially groundbreaking finding in Nature: a genetic variant in the angiotensin-converting enzyme ACE appeared to modify an individual’s risk of having a heart attack. This finding was notable at the time for the size of the study, which involved a total of over 500 individuals from four cohorts, and the effect size of the identified variant–in a population initially identified as low-risk for heart attack, the variant had an odds ratio of over 3 (with a corresponding p-value less than 0.0001).
Readers familiar with the history of medical association studies will be unsurprised by what happened over the next few years: initial excitement (this same polymorphism was associated with diabetes! And longevity!) was followed by inconclusive replication studies and, ultimately, disappointment. In 2000, 8 years after the initial report, a large study involving over 5,000 cases and controls found absolutely no detectable effect of the ACE polymorphism on heart attack risk.
The ACE story is not unique to the ACE polymorphism or to medical genetics; the problem is common to most fields of empirical science. If the sample size is small then statistically significant results must have big effect sizes. Combine this with a publication bias toward statistically significant results, plenty of opportunities to subset the data in various ways and lots of researchers looking at lots of data and the result is diminishing effects with increasing confidence, as beautifully shown in the figure.
For more see my post explaining Why Most Published Research Findings are False and Andrew Gelman’s paper on the statistical challenges of estimating small effects.
Addendum: Chris Blattman does his part to reduce bias. Will journal editors follow suit?
We’re going to see a lot more part-time employment
This is from a few weeks’ back and I had been meaning to cover it:
Wal-Mart will drop health insurance benefits for its part-time workers, the New York Times reports this morning.
Sarah Kliff offers related comment:
The [ACA] law, however, is largely silent on the subject of part-time workers, and there are no penalties for not offering them coverage.
That makes the divide between “full time” and “part time” a key distinction for the health-care law, and one the Obama administration is fine-tuning.
It will not be an easy fine tune.
Sentences to ponder
It is estimated that up to 40 percent of prescriptions go unfilled…
That is from Ezekiel J. Emanuel, here is more. I read somewhere that Zeke has a memoir under contract somewhere, but now Google fails me. Can this be true?
