Category: Medicine
US Human Experimentation Without Consent or Contract
In July 1946, 20-year-old Helen Hutchison walked into the Vanderbilt University prenatal clinic in Nashville, Tennessee. Helen found herself pregnant after her husband had returned from combat in World War II. The pregnancy, however, had not been easy. During her visit to the clinic Helen’s doctor handed her a small drink.
“What is it?” she asked.
“It’s a little cocktail,” her doctor replied. “It’ll make you feel better.”
“Well I don’t know if I should be drinking a cocktail,” she responded in jest.
“Drink it all. Drink it all down” (quoted in Welsome 1999, p. 220).Helen did as her doctor ordered.
Three months later Helen’s daughter, Barbara, was born. Not long after, Helen began to experience some frightening health problems; her face swelled, and her hair fell out. She then experienced two miscarriages, one of which necessitated 16 blood transfusions (Welsome 1999, p. 220). Baby Barbara experienced her own health problems from early childhood. She suffered from extreme fatigue and developed an autoimmune disorder and eventually skin cancer.
…Unbeknownst to Helen, she and her unborn baby had been subjects in a government-funded experiment. She was one of hundreds of women who received an experimental “cocktail” between 1945 and 1947 during one of their prenatal visits, compliments of the U.S. Atomic Energy Commission (AEC), which provided the materials (Wittenstein 2014, p. 39).
The 829 women of the Vanderbilt clinic were but a few of hundreds of thousands of individuals, mostly U.S. citizens, who would be subjected to illegal experiments and suffer human-rights violations during in the post-World War II period at the hands of scientists with funding and materials provided by the U.S. government. These experiments were meant to provide the government with information about the effects of atomic weapons on the human body to advance military capabilities in the name of “national security.”
This paper tells the story of U.S. government activities related to human experimentation after World War II.
That’s Coyne and Hall writing on Dr. Mengele, USA Style: Lessons from Human Rights Abuses in Post World War II America. It’s interesting that these immoral experiments using radiation and also agents of chemical warfare are less well known to the public than say the Tuskegee Study even though they involved far more people.
New data on marijuana legalization
That is the topic of my latest Bloomberg column, and here is one excerpt:
What do the numbers show? A new study from the Federal Reserve Bank of Kansas City offers some important keys toward an answer.
Start with the good news, or what appears to be the good news. Post-legalization, incomes in legalizing states grew by about 3%, home prices went up by 6%, and populations rose by about 2%. The researchers used appropriate statistical controls, but there is some question about causation vs. correlation. At the very least, it seems highly likely that state GDP went up: A state with legal marijuana can sell it, including to users in other states. Selling marijuana is a new business, and like any new business, it boosts the local economy.
But it is not so simple. Measures of GDP and GDP per capita are usually good metrics for human well-being — but not always. Cigarette sales, for instance, are not as beneficial for citizens as much as the initial GDP boost might indicate, because nicotine is bad for most people…
In states with legal marijuana, self-reported usage rose by 28%. Meanwhile, substance use disorders increased by 17%. Chronic homelessness went up by 35%, a possible sign that marijuana use leads to a downward financial spiral, and perhaps job loss, for many users. Arrests increased by 13%, although reported crime did not itself go up.
And in sum:
That said, these results are hardly a great advertisement for the legalization experiments. They stand in jarring contrast to what advocates promised: an end to black markets, safer marijuana and a better-protected user population. And if I may be allowed to think less like an economist for a moment, I confess I don’t feel good about a social practice that lowers effective IQ. No one smokes pot to perform better on their SATs.
I remain of two minds on the entire question.
Worth a ponder.
Jake Seliger is Dead
We all knew it was coming but it’s no less painful to learn that Jake Seliger has died. I never met Jake in person but we were pen pals? email pals? blog friends? for well over a decade. We shared an interest in speeding up drug research and development, including FDA deregulation, an interest which long preceded Jake’s cancer diagnosis. But mostly I thought he was a great writer and human being. His essays were always thoughtful and without pretense or sentimentality.
Jake’s wife, Bess Stillman is now 7 months pregnant with their daughter. Bess is an ER physician and a remarkable woman. Here is an interview with her on the infuriating difficulty of getting a patient enrolled in a clinical trial in the United States. Here is How to Say It, her gripping telling on the Moth Radio hour of how she tells people their loved ones have died. If you wonder about the title of this post, that is why. Do read How to Let Go on her last days with Jake. Sigh.
Here is Jake:
One virtue of a prolonged end is that I feel like I’ve said everything I have to say. I don’ t know that I have a favorite, but I’m fond of “I know what happens to me after I die, but what about those left behind?” Same with “How do we evaluate our lives, at the end? What counts, what matters?” I’m tempted to keep citing others, but if you scroll down into the archives you will find them. I meant to turn these essays into a memoir, but that is a project never to be completed by me. Bess assures me that she’s going to complete the project and do her best to get it published. We’ve created so much together in the process of building our life, and Bess says that doesn’t need to stop just because I’m not physically here, and that putting both our baby and our book into the world gives her immediate future the purpose that she’ll badly need.
Though having my life cut short by cancer is horrible, I’ve still in many ways been lucky. Most people never find the person who completes them, I think, and I have. I’ve been helped so much. Numerous oncologists have gone above and beyond. Many people, friends and strangers, have asked if there is anything they can do to help. The #1 thing is to support Bess and our soon-to-be-born daughter, Athena, whatever “support” may mean—the most obvious way is the Go Fund Me, as any remaining funds will go to Athena. I wish she could grow up with her father, but that is not an option. Being a single mom is hard;[1] growing up without a parent is hard; I cannot see what Athena’s future holds, except that I think and hope it will be bright, even though I will not be in it, save for the ways in which friends and family promise to keep me alive for her.
Markets in Everything: Fentanyl Precursors
Reuters: To learn how this global industry works, reporters made multiple buys of precursors over the past year. Though a few of the sales proved to be scams, the journalists succeeded in buying 12 chemicals that could be used to make fentanyl, according to independent chemists consulted by Reuters. Most of the goods arrived as seamlessly as any other mail-order package. The team also procured secondary ingredients used to process the essential precursors, as well as basic equipment – giving it everything needed to produce fentanyl.
The core precursors Reuters bought would have yielded enough fentanyl powder to make at least 3 million tablets, with a potential street value of $3 million – a conservative estimate based on prices cited by U.S. law enforcement agencies in published reports over the past six months.
The total cost of the chemicals and equipment Reuters purchased, paid mainly in Bitcoin: $3,607.18.
I don’t doubt that Reuters did what they say they did. I have trouble believing, however, that the implied profit margins are so high. A gram of cocaine costs about $160 on the street and $13 to $70 trafficked into the US and ready to sell. Thus, the street price to production cost is at most 12:1 and perhaps as low as 2.3:1. Note that this profit margin includes the costs of jail etc. I think Reuters overestimates fentanyl street prices by a factor of 2 which would still give a ratio of 415:1 which is way too high. Let’s say fentanyl sells for $1.5 million on the street then to get the ratio to a very generous 20:1 we need costs of $75,000 so my guess is that Reuters has underestimated costs by a significant amount in some manner.
Happy to receive clarification or verification from those with more expertise in the business.
I do accept Reuters point that fentanyl is cheap and easy to produce.
The whole story is excellent.
Does Income Affect Health? (an RCT)
This paper provides new evidence on the causal relationship between income and health by studying a randomized experiment in which 1,000 low-income adults in the United States received $1,000 per month for three years, with 2,000 control participants receiving $50 over that same period. The cash transfer resulted in large but short-lived improvements in stress and food security, greater use of hospital and emergency department care, and increased medical spending of about $20 per month in the treatment relative to the control group. Our results also suggest that the use of other office-based care—particularly dental care—may have increased as a result of the transfer. However, we find no effect of the transfer across several measures of physical health as captured by multiple well-validated survey measures and biomarkers derived from blood draws. We can rule out even very small improvements in physical health and the effect that would be implied by the cross-sectional correlation between income and health lies well outside our confidence intervals. We also find that the transfer did not improve mental health after the first year and by year 2 we can again reject very small improvements. We also find precise null effects on self-reported access to health care, physical activity, sleep, and several other measures related to preventive care and health behaviors. Our results imply that more targeted interventions may be more effective at reducing health inequality between high- and low-income individuals, at least for the population and time frame that we study.
That is from a new NBER working paper by
Every Stock is a Vaccine Stock, Revisited
In May 2020, I wrote a post titled Every Stock is a Vaccine Stock highlighting that the stock market reaction to good vaccine news indicated that vaccines were worth trillions and that most of this value was external to the vaccine manufacturers, meaning that the vaccine manufacturers were under-incentivized.
It’s not surprising that when Moderna reports good vaccine results, Moderna does well. It’s more surprising that Boeing and GE not only do well they increase in value far more than Moderna. On May 18, for example, when Moderna announced very preliminary positive results on its vaccine it’s market capitalization rose by $5b. But GE’s market capitalization rose by $6.82 billion and Boeing increased in value by $8.73 billion.
A cure for COVID-19 would be worth trillions to the world but only billions to the creator. The stock market is illustrating the massive externalities created by innovation. Nordhaus estimated that only 2.2% of the value of innovation was captured by innovators. For vaccine manufacturers it’s probably closer to .2%.
Who can internalize the externalities? Moderna clearly can’t because if they could then on May 18 Moderna would have increased in value by $20.52b ($4.97b+$6.82b+$8.73b) and GE and Boeing wouldn’t have gone up at all. Massive externalities.
A clever institutional investor like Blackrock or Vanguard could internalize some of the externalities by encouraging Moderna to work even faster and invest even more, even to the extent of lowering Moderna’s profits. Blackrock would more than make up for the losses on Moderna by bigger gains on other firms in its portfolio. Blackrock does indeed understand the incentives, although its unclear how much beyond jawboning they can actually do, legally.
I’d like to see more innovation in mechanisms to internalize externalities–perhaps in a pandemic vaccine firms should be given stock options on the S&P 500. Until we develop those innovations, however, the government is the best bet at internalizing the externality by paying vaccine manufacturers to increase capacity and move more quickly than their own incentives would dictate. Billions in costs, trillions in benefits.
A new paper by Acharya, Johnson, Sundaresan and Zheng formulizes this intuition. The authors combine a model of preferences in which uncertainty can be priced with an estimate of the stock market reaction to vaccine news and conclude that “ending the pandemic would have been worth from 5% to 15% of total wealth”.
One measure of the ex ante cost of disasters is the welfare gain from shortening their expected duration. We introduce a stochastic clock into a standard disaster model that summarizes information about progress (positive or negative) toward disaster resolution. We show that the stock market response to duration news is essentially a sufficient statistic to identify the welfare gain to interventions that alter the state. Using information on clinical trial progress during 2020, we build contemporaneous forecasts of the time to vaccine deployment, which provide a measure of the anticipated length of the COVID-19 pandemic. The model can thus be calibrated from market reactions to vaccine news, which we estimate. The estimates imply that ending the pandemic would have been worth from 5% to 15% of total wealth as the expected duration varied in this period.
Disappearing polymorphs
Here’s a wild phenomena I wasn’t previously aware of: In crystallography and materials science, a polymorph is a solid material that can exist in more than one crystal structure while maintaining the same chemical composition. Diamond and graphite are two polymorphs of carbon. Diamond is carbon crystalized with an isometric structure and graphite is carbon crystalized with a hexagonal structure. Now imagine that one day your spouse’s diamond ring turns to graphite! That’s unlikely with carbon but it happens with other polymorphs when a metastable (locally) stable version becomes seeded with a stable version.
The drug ritonavir originally used for AIDS (and also a component of the COVID medication Paxlovid), for example, was created in 1996 but in 1998 it couldn’t be produced any longer. Despite the best efforts of the manufacturer, Abbott, every time they tried to create the old ritonavir a new crystalized version (form II) was produced which was not medically effective. The problem was that once form II exists it’s almost impossible to get rid of it and microscopic particles of form II ritonavir seeded any attempt to create form I.
Form II was of sufficiently lower energy that it became impossible to produce Form I in any laboratory where Form II was introduced, even indirectly. Scientists who had been exposed to Form II in the past seemingly contaminated entire manufacturing plants by their presence, probably because they carried over microscopic seed crystals of the new polymorph.
Wikipedia continues:
In the 1963 novel Cat’s Cradle, by Kurt Vonnegut, the narrator learns about Ice-nine, an alternative structure of water that is solid at room temperature and acts as a seed crystal upon contact with ordinary liquid water, causing that liquid water to instantly freeze and transform into more Ice-nine. Later in the book, a character frozen in Ice-nine falls into the sea. Instantly, all the water in the world’s seas, rivers, and groundwater transforms into solid Ice-nine, leading to a climactic doomsday scenario.
Given the last point you will perhaps not be surprised to learn that the hat tip goes to Eliezer Yudkowsky who worries about such things.
Good news on Covid and your brain
Results: All six cognitive tests, measured before January 1, 2020, are significant predictors of infection status during the pandemic. The two subjective cognition measures show no significant association with infection. We replicate earlier cross-sectional findings of a negative association between COVID-19 infection and subsequent cognition. However, once accounting for baseline cognition, no significant associations are found for either the tests or the subjective measures. For three of the six cognitive tests the effects change signs.
Conclusions and relevance: We find no evidence for a negative association between COVID-19 infection and subsequent measures of cognitive functioning. The associations found in earlier studies may at least partly reflect reverse causation.
That is from a new research paper by Bas Weerman, et.al. Via the excellent Kevin Lewis.
Update on the Supervillains (maybe that’s you)
The law’s price controls will also deter companies from developing new medicines. A study I co-authored estimated that 135 fewer drugs will come to market through 2039 because of the Inflation Reduction Act. Research firm Vital Transformation’s forecast is even bleaker, predicting that the U.S. could lose 139 drugs within the next decade.
Dozens of life-sciences companies have announced cuts to their research and development pipelines because of the 2022 law. These announcements have come in earnings calls and filings with the Securities and Exchange Commission—where deliberate misstatements would expose executives to civil and criminal penalties—so they can’t be chalked up to political posturing.
That is from Tomas Philipson at the WSJ. It is worth noting this kind of academic research has not been effectively rebutted, rather what you usually hear in response is a bunch of snarky comments about Big Pharma and the like.
And to repeat myself yet again: if you are ever tempted to cancel somebody, ask yourself “do I cancel those who favor tougher price controls on pharma? After all, they may be inducing millions of premature deaths.” If you don’t cancel those people — and you shouldn’t — that should broaden your circle of tolerance more generally.
Testing for Bird Flu is Too Slow
Remember my warnings about the FDAs takeover of lab developed tests?
…Lab developed tests have never been FDA regulated except briefly during the pandemic emergency when such regulation led to catastrophic consequences. Catastrophic consequences that had been predicted in advanced by Paul Clement and Lawrence Tribe. Despite this, for reasons I do not understand, the FDA plan is marching forward but many other people are starting to warn of dire consequences.
Well the plan marched forward and here we are. Regarding tests for bird flu:
KFFNews: Clinical laboratories have also begun to develop their own tests from scratch. But researchers said they’re moving cautiously because of a recent FDA rule that gives the agency more oversight of lab-developed tests, lengthening the pathway to approval. In an email to KFF Health News, FDA press officer Janell Goodwin said the rule’s enforcement will occur gradually.
However, Susan Van Meter, president of the American Clinical Laboratory Association, a trade group whose members include the nation’s largest commercial diagnostic labs, said companies need more clarity: “It’s slowing things down because it’s adding to the confusion about what is allowable.”
One of the motivations for Operation Warp Speed and my work during the pandemic on things like advance market commitments was that firms wouldn’t invest enough in tests because diseases might fizzle out. The extreme costs of shutting down the economy, however, mean that it’s well worth paying for some tests for diseases that fizzle out if tests are ready when a disease doesn’t fizzle out.
Creating tests for the bird flu is already a risky bet, because demand is uncertain. It’s not clear whether this outbreak in cattle will trigger an epidemic or fizzle out. In addition to issues with the CDC and FDA, clinical laboratories are trying to figure out whether health insurers or the government will pay for bird flu tests.
We need a pandemic trust fund to ramp up advance market commitments when necessary.
On the plus side, I do approve of the new program to pay farmers and farm workers for testing. For example:
Friday’s incentives announcement included a $75 payment to any farm worker who agrees to give blood and nasal swab samples to the CDC.
“Bird flu” has now infected more than 50 types of mammals. To be clear, bird flu may yet fade but every potential pandemic pathogen is a test of readiness and we still are getting a C+ at best.
The Pentagon’s Anti-Vax Campaign
During the pandemic it was common for many Americans to discount or even disparage the Chinese vaccines. In fact, the Chinese vaccines such as Coronavac/Sinovac were made quickly and in large quantities and they were effective. The Chinese vaccines saved millions of lives. The vaccine portfolio model that the AHT team produced, as well as common sense, suggested the value of having a diversified portfolio. That’s why we recommended and I advocated for including a deactivated vaccine in the Operation Warp Speed mix or barring that for making an advance deal on vaccine capacity with China. At the time, I assumed that the disparaging of Chinese vaccines was simply an issue of national pride or bravado during a time of fear. But it turns out that in other countries, the Pentagon ran a disinformation campaign against the Chinese vaccines.
Reuters: At the height of the COVID-19 pandemic, the U.S. military launched a secret campaign to counter what it perceived as China’s growing influence in the Philippines, a nation hit especially hard by the deadly virus.
The clandestine operation has not been previously reported. It aimed to sow doubt about the safety and efficacy of vaccines and other life-saving aid that was being supplied by China, a Reuters investigation found. Through phony internet accounts meant to impersonate Filipinos, the military’s propaganda efforts morphed into an anti-vax campaign.
… Tailoring the propaganda campaign to local audiences across Central Asia and the Middle East, the Pentagon used a combination of fake social media accounts on multiple platforms to spread fear of China’s vaccines among Muslims at a time when the virus was killing tens of thousands of people each day. A key part of the strategy: amplify the disputed contention that, because vaccines sometimes contain pork gelatin, China’s shots could be considered forbidden under Islamic law.
…To implement the anti-vax campaign, the Defense Department overrode strong objections from top U.S. diplomats in Southeast Asia at the time, Reuters found. Sources involved in its planning and execution say the Pentagon, which ran the program through the military’s psychological operations center in Tampa, Florida, disregarded the collateral impact that such propaganda may have on innocent Filipinos.
“We weren’t looking at this from a public health perspective,” said a senior military officer involved in the program. “We were looking at how we could drag China through the mud.”
Frankly, this is sickening. The Pentagon’s anti-vax campaign has undermined U.S. credibility on the global stage and eroded trust in American institutions, and it will complicate future public health efforts. US intelligence agencies should be banned from interfering with or using public health as a front.
Moreover, there was a better model. It’s often forgotten but the elimination of smallpox from the planet, one of humanities greatest feats, was a global effort spearheaded by the United States and….the Soviet Union.
…even while engaged in a pitched battle for influence across the globe, the Soviet Union and the United States were able to harness their domestic and geopolitical self-interests and their mutual interest in using science and technology to advance human development and produce a remarkable public health achievement.
We could have taken a similar approach with China during the COVID pandemic.
More generally, we face global challenges, from pandemics to climate change to artificial intelligence. Addressing these challenges will require strategic international cooperation. This isn’t about idealism; it’s about escaping the prisoner’s dilemma. We can’t let small groups with narrow agendas and parochial visions undermine collaborations essential for our interests and security in an interconnected world.
Enhancing FDA Information Sharing for Neglected Tropical Diseases
Many countries look to the US FDA for guidance on approval decisions. In fact the FDA will sometimes receive and evaluate drugs and vaccines whose primary market is in less developed countries. Fexinidazole, for example, is a drug for treating African trypanosomiasis, i.e. sleeping sickness. We don’t get many cases of sleeping sickness in the US but there are many such cases in the Democratic Republic of Congo.
Thus, the US FDA is providing a useful service, both to US pharmaceutical firms and especially to developing countries. That’s great. But Jacob Trefethen of OpenPhil notes that for odd bureaucratic and legal reasons we redact a lot of information that could be useful to the countries that actually will use these treatments. Here, for example, is an excerpt from the approval decision for Fexinidazole:

What’s especially strange here is that as far as Trefethen, or I, can tell, no one wants this! The FDA has no reason to hide this information, the company submitting the proposal surely wants as much information as possible sent to the countries where they will ultimately need to get approval (remember this is successful applications!) and the medical agencies in the developing countries would like to get context to have confidence in the FDA’s decisions. Instead, it seems that these drugs are getting caught in rules intended to protect pharmaceutical firms in other contexts. Thus, Trefethen makes two suggestions:
let’s create a track for products on the Neglected Tropical Disease list, sharing assessments with few or no redactions with the WHO Pre-Qualification (PQ) system, and allow PQ to share those documents further with regulators in partner countries.
Such an approval track already exists in the EU:
[The EU] have an approval track for products that are mostly going to be used elsewhere. If you apply using that track, they loop in regulators from those countries too. They share the documents assessing your clinical data and inspecting your manufacturing site with the WHO prequalification (PQ) team – the team whose stamp of approval speeds things up for many countries with less experienced national regulators. Gavi and the Global Fund need a product to be prequalified in order to buy it through the UN procurement agencies (e.g. UNICEF, for children’s vaccines).
Even without an approval track there are other small changes in priority and emphasis that could improve information sharing. The FDA is not unaware of these information sharing issues, for example, and there are procedures in place for confidentiality agreements with other countries. Trefethen suggests these could be given greater priority.
FDA leadership should set aggressive goals to complete more two-way Confidentiality Commitments with lower- and middle-income country regulators.
Extend the scope of existing commitments, when they’re limited, to allow sharing in more areas – especially related to drug approvals.
Extend 708(c) authority to more country agreements, not just those with European countries, to allow sharing of full documents that include trade secrets.
I’ve long advocated for peer approval, Trefethen gets into the weeds to point to specific ideas to make this a more useful idea, especially for developing countries. See Trefethen for more ideas!
Fauci Didn’t Test
I am not a Fauci hater but I think this criticism of Facui from epidemiologist and oncologist Vinay Prasad hits the mark:
Lockdown was specifically advocated for by Anthony Fauci (‘15 days to stop the spread’/ ‘hunker down’/ ‘shelter in place’), and Fauci would go on to make hundreds of other specific policy recommendations. Although he initially rejected it, by April 2020, he recommended community cloth masking to slow the coronavirus (an intervention for which we now have randomized data showing it doesn’t work).
Fauci opposed Ron DeSantis in numerous TV interviews in spring 2020 when DeSantis reopened schools. He called school reopening reckless— though it was widely embraced in western Europe at the time, and now clearly the correct policy choice.
Fauci supported vaccine mandates and border closure. He repeated the false statement that 6ft of social distancing had an empirical basis. Many in the media and medicine think criticizing him is unfair— he did the best he could with what he knew at the time—but it is fair to criticize a scientist who presented his views as facts when they were at best speculation. And, moreover, there is one criticism that no one can deny:
Although he was director of the NIAID, and although he controlled a 5 billion dollar infectious disease research budget, he chose to launch, fund and conduct precisely ZERO randomized trials of non-pharmacologic interventions.
Hat tip: MD.
The Marginal Revolution Theory of Innovation
A FDA panel voted against approving MDMA (ecstasy) for post-traumatic stress disorder. Putting aside the specifics of the case, I was vexed by this statement on innovation from one of the experts voting no:
“I absolutely agree that we need new and better treatments for PTSD,” said Paul Holtzheimer, deputy director for research at the National Center for PTSD, a panelist who voted no on the question of whether the benefits of MDMA-therapy outweighed the risks.
“However, I also note that premature introduction of a treatment can actually stifle development, stifle implementation and lead to premature adoption of treatments that are either not completely known to be safe, not fully effective or not being used at their optimal efficacy,” he added.
A textbook example of making the perfect the enemy of the good. But the problem is even worse. Holtzheimer seems to think that treatments spring from the lab perfectly formed like Athena springing from the brow of Zeus. Indeed, Holtzheimer suggests that treatments should be kept in the lab until they are perfect. News flash: there are no perfect treatments–no drug or device in use today is completely known to be safe, fully effective, and used at its optimal efficacy. Not one. If we follow Holtzheimer’s counsel, we will never approve a new drug.
Innovation is a dynamic process; success rarely comes on the first attempt. The key to innovation is continuous refinement and improvement. A firm with sales gains greater resources to invest in further research and development. Additionally, they benefit from customer feedback, which provides valuable insights for enhancing their products and processes. Learning by doing requires doing. But if imperfect treatments are never approved, scientists often don’t return to the lab to refine and improve them. Instead, the project dies. Thus, when considering innovation today, it’s essential to think about not only the current state of technology but also about the entire trajectory of development. A treatment that’s marginally better today may be much better tomorrow.
Small steps toward a much better world.
The NIH Doesn’t Fund Small Crappy Trials
A nice catch by Max at Maximum Progress:
[A common critique] is that the NIH funds too many “small crappy trials.” That quote is from a FDA higher up, but the story has been repeated by many others…I downloaded all of the clinical trial data from ClinicalTrials.gov to find out….The median NIH funded trial has 48 participants while the median industry funded trial has 67. The average NIH funded trial has 288 participants while the average industry trial has 335 and the average “Other” funded trial (mostly universities and the associated hospitals) has 923 participants.
By median or by average NIH trials are the smallest out of all the funders. This seems to confirm the “small crappy trials” narrative
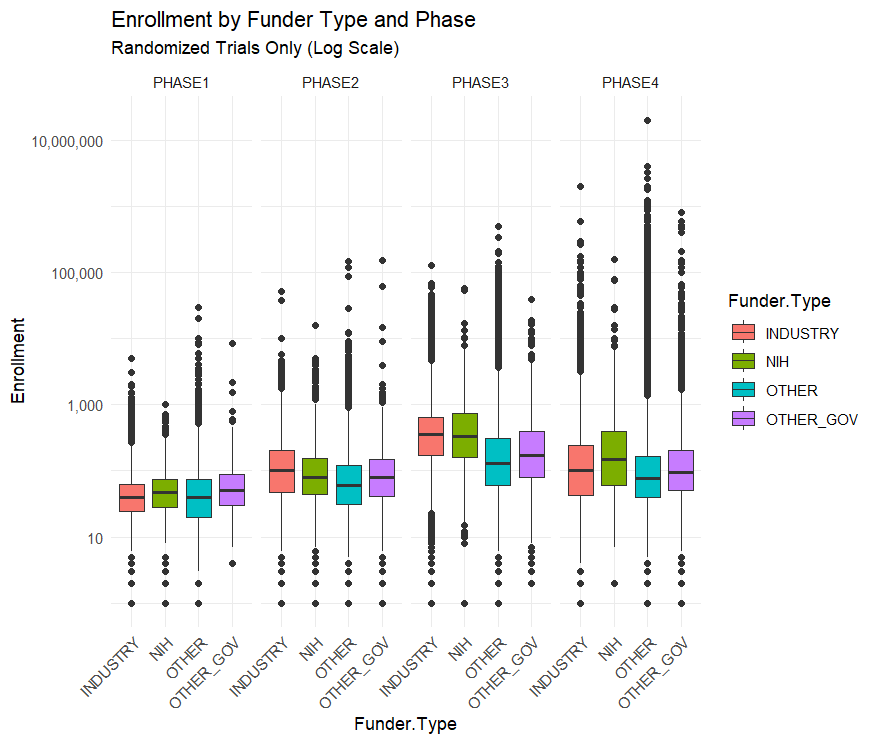
…This narrative is reversed, however, when you split up the trials by phase.
Across all trials NIH funded ones are the smallest, but within each phase NIH trials are the largest or second largest. Their overall small enrollment average is just due to the fact that they fund more Phase I trials than Phase III. But NIH Phase I trials have a bigger sample size than industry funded trials on average.
This is an example of Simpson’s Paradox in the wild!
Arguing that the NIH should stop funding unusually small trials is easy but arguing that they should shift from funding the Phase I trials closest to basic research towards later stage trials is less clear.
The NIH’s clinical trial strategy is certainly not perfect and improving it is valuable. But a systematic bias towards “small crappy trials” doesn’t really seem like it’s an important problem facing the NIH.