Category: Economics
Some simple spatial analytics of Cape Town
Rio de Janeiro let its hillsides be filled in with lower-cost dwellings. The result was a significant increase in the crime rate. On the more positive side of the ledger, upward mobility increased too. If you live in a decent favela, you can get to a downtown job with not too much difficulty, albeit with some travel risk. Note however that some of those jobs include “theft.”
Cape Town has not filled in its hillsides, and you see empty, valuable land all over the place. The townships have remained remarkably segregated, both racially and spatially. The nicer parts of Cape Town also have remained relatively safe, both for whites and for upper class blacks.
One secondary consequence of this equilibrium is very high unemployment in the townships, staggeringly high in fact. It is expensive to get from most of the townships to a job in the nicer part of town. For South Africa as a whole, GPT Pro reports:
OECD reports that around 70% of discouraged jobseekers cite location as the main obstacle to looking for work, and that commuting can absorb up to 37% of post-tax income for the lowest quintile, or up to 80% once time costs are included. The World Bank estimate is even harsher for the poorest households: up to 85% of daily income once the opportunity cost of time is counted. In effect, many low-wage jobs are too costly to search for, reach, or keep.
And see this link. Young male workers in particular find it hard to get the experience that would enable them to prove themselves reliable and then keep on climbing a skills ladder. So they stay in the townships, maybe engage in some black or gray market labor, and collect some welfare payments. They also might commit crimes against each other.
Which in turn makes the notion of filling in the hillside with low-cost housing all the less appealing.
It is difficult to solve the problems of South Africa.
Addendum: Note also that South African agriculture is capital-intensive, as you might expect from a wealthier country. So subsistence agriculture is less of an option here, compared to many other African nations, and that leads to all the more overcrowding in the poorly located townships.
Studying with Ludwig Lachmann
Since I am in South Africa, I am reminded of my time studying with Ludwig Lachmann, the South African economist from University of the Witwatersrand. I was seventeen, and Lachmann teaching a graduate seminar at New York University. Someone (Richard Ebeling maybe?) had told me he was interesting, so I wanted to sit in on the seminar. I showed up, introduced myself to Lachmann, and asked if I could listen to the lectures. I obviously did not belong, but he was very gracious and said yes of course. He wore a suit and tie, had a very Old World manner, and he had been a Jewish refugee from Germany. He was 73 or so at the time, this was 1979.
His manner of speaking was very distinctive. Of course I now recognize the South African accent, but there is more to it than that.
Lachmann was best known for his connections to the Austrian School, as he was visiting at the NYU Austrian program at the time, under the aegis of Israel Kirzner. Nonetheless Austrian economics was not what I learned in the seminar.
On the first day, I heard plenty about Sraffa and Garegnani, and all that was new (and fascinating to me). Lachmann had studied with Werner Sombart, so I learned about the German historical school as well.
Lachmann also was my first teacher who made sense of Keynes for me, moving me away from obsessions with the hydraulic IS-LM interpretations of the General Theory. He flirted with views of cost-based pricing, brought me further into the kaleidic world of G.L.S. Shackle, and he insisted that a market economy had no overall tendency toward the constellation of a general equilibrium of prices and quantities. (He did believe that most though not all individual markets tended to equilibrate.) He inveighed against W.H. Hutt’s interpretation of Say’s Law, of course some of you here will know that Hutt also was South African. I kept on trying to read Hutt, to see if I could defend him against Lachmann’s critiques. I also imbibed Hutt’s economic critique of apartheid.
Lachmann did not talk about South Africa, other than to mention how long the journey to New York was. You may know that Israel Kirzner, another early mentor of mine, had South African roots as well. He also did not talk about South Africa.
“South African economics,” if you wish to call it that, played a significant role in my early intellectual development.
To this day, when I think about the economics of AI, and many other matters, Lachmann’s book Capital and its Structure is one of my go-to inspirations.
And I am still grateful to Lachmann for letting “a kid” sit in on his class. I paid avid attention.
Why is the USDA Involved in Housing?!
In yesterday’s post, The 21st Century ROAD to Housing Act, I wrote that Trump’s Executive Order “cuts off institutional home investors from FHA insurance, VA guarantees and USDA backing…”. The USDA is of course the United States Department of Agriculture. In the comments, Hazel Meade writes:
USDA? Wait, what????
Why is the USDA in any way involved in housing financing?
Are we humanly capable of organizing anything in a rational way?
It’s a good question. The answer is a great illustration of the March of Dimes syndrome. The USDA got involved with housing in the late 1940s with the Farmers Home Administration. The original rationale was to support farmers, farm workers and agricultural communities with housing assistance on the theory that housing was needed for farming and the purpose of the USDA was to improve farming. Not great economic reasoning but I’ll let it pass.
Well U.S. farm productivity roughly tripled between 1948 and the 1990s as family farms became technologically sophisticated big businesses. So was the program ended? Of course not. Over time the program subtly shifted from farmers to “rural communities”–the shift happened over decades although it was officially recognized in 1994 when the Farmers Home Administration was renamed the Rural Housing Service. Today rural essentially means low population density which no longer has any strong connection to agriculture.
So that’s the story of how the US Department of Agriculture came to run a roughly $10 billion annual housing program for non-farmers in non-agricultural communities. And how does it do this? By supporting no-money-down direct lending and a 90 percent guarantee to approved private lenders. Lovely.
It’s a small program in the national totals, but an amusing example of the US government robbing Peter to pay Paul and then forgetting why Paul needed the money in the first place.
The 21st Century ROAD to Housing Act
The 21st Century ROAD to Housing Act appears likely to pass the Senate. The bill contains some genuinely good ideas alongside some very popular—but bonkers ideas.
Let’s start with the good ideas.
The bill would streamline NEPA review for federally supported housing, primarily by expanding categorical exclusions. Federal environmental review does impose real costs and delays on housing construction, so reducing unnecessary review is a step in the right direction. The gains will probably be modest—most housing regulation occurs at the state and local level—but removing friction is good.
The bill would also deregulate manufactured housing by eliminating the permanent chassis requirement and creating a uniform national construction and safety standard. The United States once built far more factory-produced housing; in the early 1970s, by some accounts a majority of new homes were factory-built (mobile or modular). Long-run productivity growth in housing almost certainly requires greater use of factory construction. Land-use regulation remains the dominant constraint on supply, but enabling scalable manufacturing is still welcome.
Another interesting provision involves Community Development Block Grants (CDBG). The bill allows CDBG funds to be used for building new housing rather than being largely restricted to rehabilitation of existing housing. More federal spending is not automatically appealing, but the bill adds an unusual incentive mechanism.
The bill creates a tournament for CDBG allocations. Localities that exceed the median housing growth improvement rate among eligible CDBG recipients receive bonus funding. Those below the median face a 10 percent reduction. The key feature is that the penalties fund the bonuses, so the system reallocates money rather than expanding spending.
This is a clever design. It creates competition among localities and benchmarks them against peers rather than against a fixed national target. In effect, the program rewards relative improvement rather than absolute performance—a classic tournament structure. (See Modern Principles for an introduction to tournament theory!).
Ok, now for the popular but bonkers ideas. Section 901 (“Homes are for People, Not Corporations”) restricts the purchase of new single-family homes by large institutional investors. Elizabeth Warren is a sponsor of the bill but this section was driven almost entirely by President Trump. Trump passed an Executive Order, Stopping Wall Street from Competing With Main Street Home Buyers, that cuts off institutional home investors from FHA insurance, VA guarantees, USDA backing, Fannie/Freddie securitization and so forth. The bill goes further by imposing a seven-year mandatory divestiture rule, forcing institutional investors to convert rental homes to owner-occupied units after seven years.
No one objects to institutional investors owning apartment buildings. But when the same investors own single-family homes, it breaks people’s brains. Consider how strange the logic sounds if applied elsewhere:
…a growing share of apartments, often concentrated in certain communities, have been purchased by large Wall Street investors, crowding out families seeking to buy condominiums.
Apartments are fine, hotels are fine, but somehow a corporation owning a single family home is un-American. In fact, the US could do with more rental housing of all kinds! Why take the risk of owning when you can rent? Rental housing improves worker mobility. When foreclosures surged after 2008 and traditional buyers disappeared, institutional investors stepped in and absorbed distressed supply — helping stabilize markets. Who plays that role next time?
Institutional investors own only a tiny number of homes, so even if this were a good idea it wouldn’t be effective. But it’s not a good idea, it’s just rage bait driven by Warren/Trump anti-corporate rhetoric.
What does “Homes are for People, Not Corporations” even mean?–this is a slogan for the Idiocracy era. “Food is for People, Not Corporations,” so we should ban Perdue Farms and McDonald’s?
How frequent are price bubbles?
We examine the historical frequency of stock market booms, crashes, and bubbles in the United States from 1792 to 2024 using aggregate market data and industry-level portfolios. We define a bubble as a large boom followed by a crash that reverses the market’s prior gains. Bubbles are extremely rare. We extend the industry-level analysis of Greenwood, Shleifer, and You (2019) through 2024 and replicate their findings out of sample using Cowles Commission industry data from 1871 to 1938. Booms do not reliably predict crashes, but they do predict higher subsequent volatility, increasing the likelihood of both large gains and large losses.
That is from a new NBER working paper by William N. Goetzmann, Otto Manninen, and James Tyler.
Advantageous Selection
I tweeted: Should I be worried or reassured that my taxi driver isn’t wearing a seat belt? An econ puzzle.
Most replies said I should be worried. I think that is correct and it reveals something of importance. First note that there is an incentive and a selection effect. All else equal, a driver without a seat belt should drive more carefully—that’s the rational response to increased personal risk. But drivers who forgo seat belts are probably more risk-loving or less safety-conscious across many dimensions. I think the replies were correct, the second effect, the selection effect, dominates: be worried.
What makes this an economics puzzle is that it reveals a failure of the standard adverse selection story. Adverse selection predicts that if someone wants to buy a lot of life insurance, the seller should be suspicious—fearing the buyer knows something about their own health that the seller doesn’t. Unusually healthy people, by the same logic, should buy less life insurance.
Notice the parallel to the taxi driver: the driver is buying less insurance (by not wearing a seat belt) and so, by adverse selection logic, should be the safer type. But that’s exactly backwards.
In reality, people who buy a lot of life insurance tend to be the kind of people who take care of themselves on many margins—they eat well, exercise, go to the doctor. Insurers know this, which is why the per-unit price of life insurance falls with quantity. Big buyers are the good risk, not the bad one.
The taxi driver puzzle is a clean real-world case where the selection effect runs opposite to what adverse selection theory predicts. Adverse selection theory is correct that information asymmetries can challenge markets but it’s often not obvious which way the asymmetry runs (who know more about your life expectancy, you or an insurance company with millions of data points?). Moreover, preferences and norms can make the selection run the opposite way so be worried about the taxi driver without a seat belt and be happy when someone demands a lot of life insurance.
Academic journals and AI bleg
Given the rapid pace of advancement of AI, how should academic journals adapt to these changes? One issue might be an excess of submissions, but what other questions should be considered here? Which reforms should be made?
Your thoughts would be most welcome.
A market-based officer retention system?
The Army is launching a new Warrant Officer Retention Bonus Auction. This initiative introduces a market‑based approach to retaining senior technical talent while ensuring responsible stewardship of taxpayer dollars. The program represents a shift from traditional, fixed‑rate bonuses to a more flexible, market-driven system.
The structure is designed to make the best strategy straightforward—bid your true value. Eligible warrant officers will submit a confidential bid indicating the minimum monthly bonus they would be satisfied receiving in exchange for a six‑year Active‑Duty Service Obligation. Overbidding increases the risk of missing out on a bonus, while underbidding could result in commitment to a lower rate. Army leadership believes the system rewards transparency and encourages officers to carefully consider the compensation that would make them comfortable with continued service.
“The goal is simple. Reward as many qualified Warrant Officers as possible with the most competitive bonus the budget allows,” said Lt. Col. Tim Justicz, an Army economist who helped design the program.
Once bids are submitted, the Army will determine a single market‑clearing bonus rate that retains the maximum number of qualified warrant officers within the available budget. Every warrant officer whose bid falls at or below that rate will receive the same bonus amount. This means that warrant officers who bid lower than the final rate will still receive the higher, market‑determined bonus.
Here is more, via Charles Klingman.
The Hidden Cost of Hard-to-Fire Labor Laws: Why European Firms Don’t Take Risks
In our textbook, Modern Principles, Tyler and I write:
Imagine how difficult it would be to get a date if every date required marriage? In the same way, it’s more difficult to find a job when every job requires a long-term commitment from the employer.
In two new excellent pieces, Brian Albrecht and Pieter Garicano extend this partial equilibrium aphorism with some general equilibrium reasoning. Here’s Albrecht:
[I]magine there is a surge for Siemens products. Do you hire a ton of workers to fill that demand? No, you’re worried about having to fire them in the future but being stuck until they retire.
But it’s even worse than that…..[suppose Siemens does want to hire] where is Siemens getting those workers from?…Not only is it a problem for Siemens that they won’t be able to fire people down the road, the fact that BMW doesn’t fire anyone means you can’t hire people.
Garicano has an excellent piece, Why Europe doesn’t have a Tesla, with lots of detail on European labor law:
Under the [German] Protection Against Dismissal Act, the Kündigungsschutzgesetz, redundancies over ten employees must pass a social selection test (Sozialauswahl). Employers cannot choose who leaves: they must rank employees by age, years of service, family maintenance obligations, and degree of disability, and then prioritize dismissing those with the weakest social claim to the job. If someone is dismissed for operational reasons but the company posts a similar job elsewhere, the dismissal is usually invalid.
Disabled employees can be dismissed only with the approval of the Integration Office (Integrationsamt), a public body. The office will weigh the employer’s reasons, whether they have taken sufficient steps to integrate the employee, and whether they could be redeployed elsewhere in the organization. Workers who also become caregivers cannot be dismissed at all for up to two full years after they tell their bosses they fulfill that role.
As a company becomes larger and tries to let more workers go at once these difficulties increase. In many European countries, companies with more than a certain number of workers – 50 in the Netherlands, 5 in Germany – are obliged to create a works council, which represents employees and, in some countries, must give its approval to decisions the employer wants to make regarding its employees, including layoffs or pay rises or cuts.
…Companies that are allowed to fire someone and can afford to pay the severance costs have to wait and pay additional fees. Collective dismissal procedures in Germany start after 30 departures within a month; once triggered they require further negotiations with the works council, a waiting period, and the creation of a ‘social plan’ with more compensation for departing workers. When Opel shut down its Bochum factory in Germany, it reached a deal with the works council to spend €552 million on severance for the 3,300 affected employees. This included individual payments of up to €250,000 and a €60 million plan to help workers find new jobs.
Now what is the effect of regulations like this? Well obviously the partial equilibrium effect is to reduce hiring but in addition Garicano notes that it changes what sorts of firms are created in the first place. If you are worried about being burdened by expensive dismissal procedures, build a regulated utility with captive government contracts, not a radical startup with a high probability of failure.
Rather than reduce hiring in response to more expensive firing, companies in Europe have shifted activity away from areas where layoffs are likely. European workers are for sure, solid work only. This works well in periods of little innovation, or when innovation is gradual. The continent, however, is poorly equipped for moments of great experimentation.
…Europe’s companies have immense, specialized knowledge [due to retained workforces, AT]. The problems happen when radical innovation is needed, as in the shift from gasoline to electric vehicles. The great makers of electric cars have either been new entrants, like Tesla and BYD, or old ones who have had their insides stripped, like MG.
..If Europe wants a Tesla, or whatever the Tesla of the next decade will turn out to be, it will need a new approach to hiring and firing.
Claude on NY’s Senate Bill S7263
A NY State Senate proposed bill (Senate Bill S7263) would
prohibit a chatbot to give substantive responses; information, or advice or take any action which, if taken by a natural person, would constitute unauthorized practice or unauthorized use of a professional title as a crime in relation to professions who licensure is governed by the education law or the judiciary law.
Claude, what do you think of the legal logic of this bill?
The legal logic is shaky. The bill’s operative test asks whether a chatbot’s output, “if taken by a natural person, would constitute a crime” under New York’s unauthorized practice statutes. But those statutes set a high bar — mere advice-giving by a layperson is not criminal; what’s prohibited is holding yourself out as a licensed professional while charging fees. Your neighbor who happens to be a doctor can tell you what he thinks your rash is. A retired lawyer can walk you through a lease. None of that is a crime. So either the bill is mostly toothless — most AI responses wouldn’t meet the criminal threshold — or courts will interpret “substantive advice” far more expansively than the underlying statutes warrant, effectively creating a new and harsher legal standard for AI that applies to no human equivalent. Neither outcome reflects good lawmaking, and the ambiguity will systematically over-deter, pushing operators to sanitize outputs well beyond what the statute actually requires.
Claude, who will be hurt by this bill?
The deepest problem is who gets hurt. The populations with the most to gain from AI-assisted professional guidance are precisely those who cannot afford lawyers, doctors, or therapists — the tenant trying to understand an eviction notice, the rural patient triaging symptoms, the small business owner reviewing a contract. For these users, the choice the bill actually creates is not “AI advice versus licensed professional advice”; it’s “AI advice versus no advice at all.” A watered-down chatbot that responds to every medical or legal question with a referral to a licensed professional is not a safety feature — it’s a luxury tax on information, paid disproportionately by people with the fewest alternatives. New York should be asking how to ensure AI advice is accurate and clearly disclosed, not how to suppress it on behalf of incumbents who’d prefer less competition.
Thanks Claude. Where did you learn this excellent analysis?
Public choice theory is part of my general training on economics and political science literature — Buchanan, Tullock, Olson, and the broader tradition are well-represented in the texts I was trained on.
But I’d be remiss not to note that you’re at the home institution of public choice. The Buchanan House is literally on your campus, and the tradition Buchanan and Tullock built at GMU is probably the most direct intellectual ancestor of the kind of analysis I was applying to this bill — concentrated benefits, diffuse costs, regulatory capture, rent-seeking by incumbent professionals. That framework is so natural for analyzing occupational licensing legislation that it almost applies itself.
If anything, my read of S7263 is pretty much a straightforward public choice story: organized professional associations with strong lobbying presence get statutory protection written in the language of consumer welfare, while the costs fall on millions of unorganized users who will never know what information they didn’t receive. Buchanan would have recognized it immediately.
The value of good high schools
Improving education and labor market outcomes for low-income students is critical for advancing socioeconomic mobility in the United States. We use longitudinal data on five cohorts of 9th grade students to explore how Massachusetts public high schools affect the longer-term outcomes of students, with a special focus on students from low-income families. Using detailed administrative and student survey data, we estimate school value-added impacts on college outcomes and earnings. Observationally similar students who attend a school at the 80th percentile of the value-added distribution instead of a school at the 20th percentile are 11% more likely to enroll in college, are 31% more likely to graduate from a four-year college, and earn 25% (or $10,500) more annually at age 30. On average, schools that improve students’ longer-run outcomes the most are those that improve their 10th grade test scores and increase their college plans the most.
That is from a new NBER working paper by
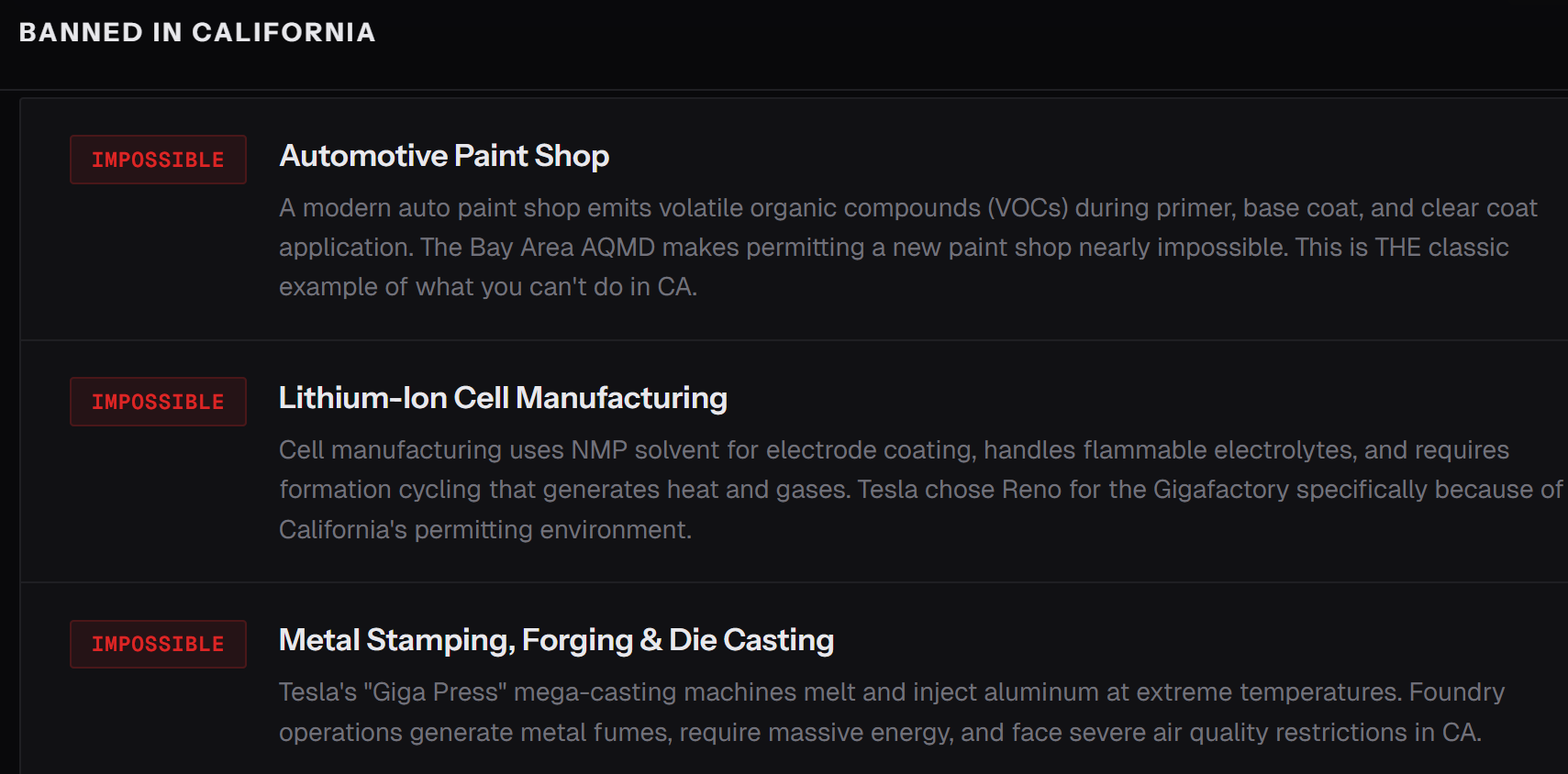
Banned in California
California cannot permit the construction of a smartphone factory, an electric car plant, or a Navy destroyer shipyard. Not won’t — can’t. The regulatory environment makes it effectively impossible to build new semiconductor fabs, automotive paint shops, battery gigafactories, or steel foundries.
Tesla didn’t put its Gigafactory in Nevada out of affection for Reno. General Dynamics NASSCO in San Diego can build destroyers only because it’s been grandfathered in since 1960. If it closed tomorrow, it could not be rebuilt.
I get tired at all the discussion of tariffs and industrial policy and manufacturing. All of it is BS in comparison to the basics. We have the met the enemy and the enemy is us. Our future is in our hands. Is that optimistic or pessimistic? Either way complaining about China won’t fix our problems.
Deflating macroeconomics?
We use long-run annual cross-country data for 10 macroeconomic variables to evaluate the long-horizon forecast distributions of six forecasting models. The variables we use range from ones having little serial correlation to ones having persistence consistent with unit roots. Our forecasting models include simple time series models and frequency domain models developed in Müller and Watson (2016). For plausibly stationary variables, an AR(1) model and a frequency domain model that does not require the user to take a stand on the order of integration appear reasonably well calibrated for forecast horizons of 10 and 25 years. For plausibly non-stationary variables, a random walk model appears reasonably well calibrated for forecast horizons of 10 and 25 years.
That is from a new NBER working paper by Kurt G. Lunsford and Kenneth D. West. If you do not know macro, here is a GPT translation in plainspeak. And this new paper suggests macro shocks do not matter that much.
Chaos and Misallocation under Price Controls
My latest paper, Chaos and Misallocation under Price Controls, (with Brian Albrecht and Mark Whitmeyer) has a new take on price controls:
Price controls kill the incentive for arbitrage. We prove a Chaos Theorem: under a binding price ceiling, suppliers are indifferent across destinations, so arbitrarily small cost differences can determine the entire allocation. The economy tips to corner outcomes in which some markets are fully served while others are starved; small parameter changes flip the identity of the corners, generating discontinuous welfare jumps. These corner allocations create a distinct source of cross-market misallocation, separate from the aggregate quantity loss (the Harberger triangle) and from within-market misallocation emphasized in prior work. They also create an identification problem: welfare depends on demand far from the observed equilibrium. We derive sharp bounds on misallocation that require no parametric assumptions. In an efficient allocation, shadow prices are equalized across markets; combined with the adding-up constraint, this collapses the infinite-dimensional welfare problem to a one-dimensional search over a common shadow price, with extremal losses achieved by piecewise-linear demand schedules. Calibrating the bounds to stationlevel AAA survey data from the 1973–74 U.S. gasoline crisis, misallocation losses range from roughly 1 to 9 times the Harberger triangle.
Brian has a superb write up that makes the paper very accessible. Unfortunately, the paper is timely and relevant.
New results on the economic costs of climate change
I promised you I would be tracking this issue, and so here is a major development. From the QJE by Adrien Bilal and Diego R Känzig::
This paper estimates that the macroeconomic damages from climate change are an order of magnitude larger than previously thought. Exploiting natural global temperature variability, we find that 1○C warming reduces world GDP by over 20% in the long run. Global temperature correlates strongly with extreme climatic events, unlike country-level temperature used in previous work, explaining our larger estimate. We use this evidence to estimate damage functions in a neoclassical growth model. Business-as-usual warming implies a present welfare loss of more than 30%, and a Social Cost of Carbon in excess of $1,200 per ton. These impacts suggest that unilateral decarbonization policy is cost-effective for large countries such as the United States.
Here is an open access version. You may recall that earlier estimates of climate change costs were more like a five to ten percent welfare loss to the world. I do not however find the main results here plausible. The estimation is extremely complicated, and based on the premise that a higher global temperature does more harm to a region than a higher local temperature. And are extreme events a “productivity shock,” or a one-time resource loss that occasions some Solow catch-up? Is the basic modeling consistent with the fact that, while the number of extreme storms may be rising, the number of deaths from those same storms is falling over time? Lives lost are not the same as economic costs, but still the capacity for adjustment seems considerably underrated. What about the effects to date? The authors themselves write: “According to our counterfactual, world GDP per capita would be more than 20% higher today had no warming occurred between 1960 and 2019.” I absolutely do not believe that claim.
In any case, here is your update. To be clear, I do absolutely favor the development of alternative, less polluting energy sources.